Intracranial tumors (Brain tumors) or space occupying lesions of the brain account for an important part of all neoplasm’s of the body, their incidence ranging from 10-15% of all neoplasm’s of the body. These involve both sexes and can occur at all age groups though some primarily occur in childhood. Intracranial tumors (Brain tumors) are classified into primary and secondary.
1. Primary tumors
(a) Glioma, glioblastoma, Astrocytoma, oligodendroglioma, ependymoma, medulloblastoma.
(b) Meningioma, neurofibroma
(c) Tumors arising from nerve sheaths –schwanoma,
(d) Pituitary tumors
(e) Infective granulorna cysticercosis.
(f) Craniopharyangiornas
(g) Blood vessel turnouts
(h) Cholesteatornata berculoma,
2. Secondary tumors
Metastases from growths in the body like breast, stomach, prostate, thyroid, kidney etc.
All these growths produce symptoms depending on the nature of lesion, rate of growth (whether slow or rapid growing). In children the symptoms develop more rapidly as the Intracranial tumors (Brain tumors) in them are more malignant. In children the common form of tumor is a medulloblastoma or nenroblastoma while in adults astrocytoma or glioblastoma are the most common type of primary tumors.
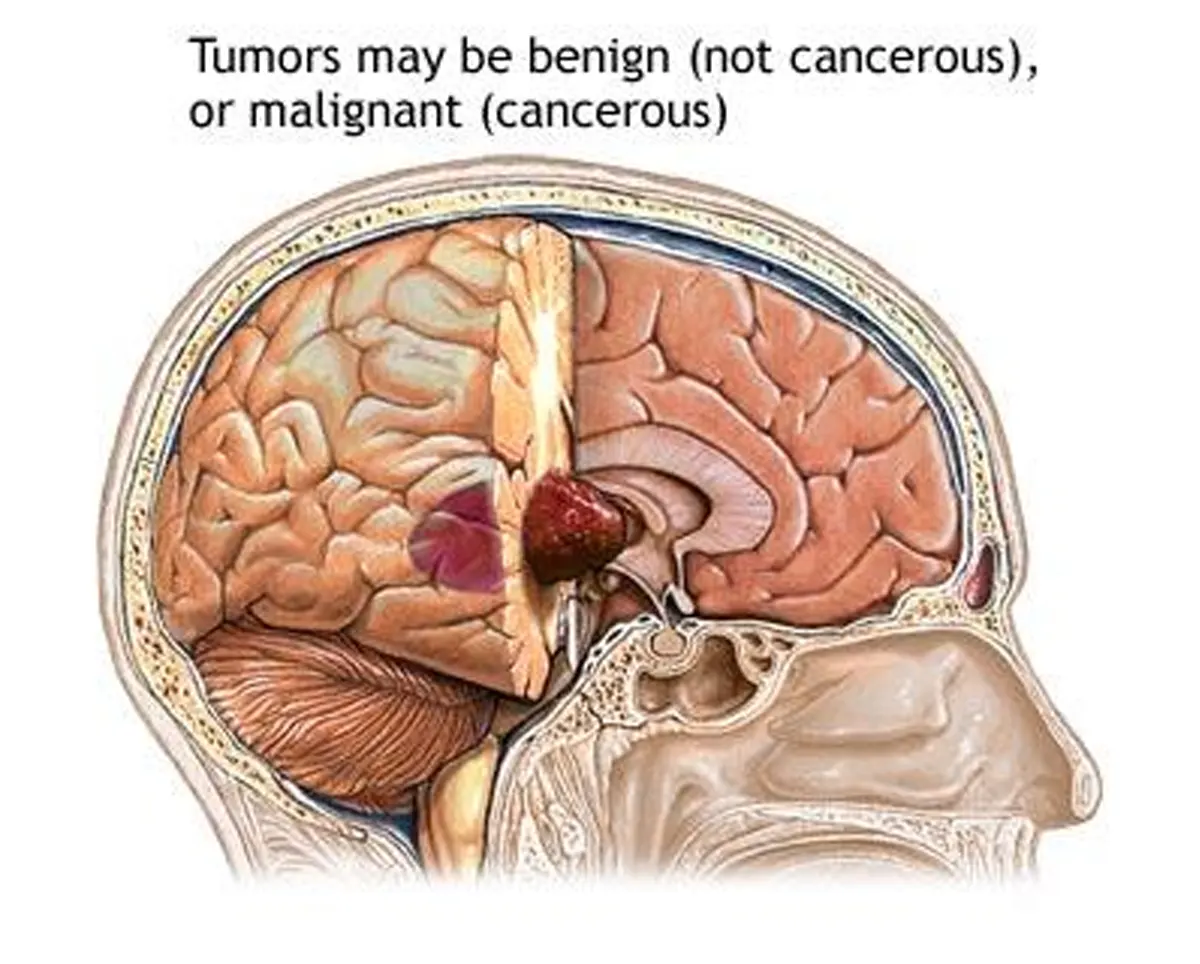
Clinical manifestations
Clinical features depend to a large extent on the rate of growth. In some the growth is slow and the tumor may remain quiescent for years without producing any symptoms while in other case the growth of the Intracranial tumors (Brain tumors) is rapid leading to fatal termination in a short period.
One of the earliest sign of space occupying lesion of the brain is raised intracranial tension and the degree to which it increases is variable depending on the growth of the tumor, its bulk and its interference with the free flow of CSF in the ventricular system. Site of the tumor also is important. Tumor of the frontal lobe may attain considerable size before symptoms develop.
The general manifestations include Headache, vomiting, giddiness, mental drowsiness, seizures, diplopia, alterations in the pulse rate and blood pressure, nasal irritation and pupil edema.
Headache
It is one of the earliest and constant symptoms. It varies from a sense of fullness to a dull constant pain with paroxysms of agonizing pain. It occurs most commonly on first waking in the morning or during night. It is often referred to the frontal or occipital region depending on the site of growth. Intracranial tumors (Brain tumors) situated anteriorly produce frontal and retro orbital pain while, patients with posterior fossa tumors complain of occipital, sub occipital or retro auricular pain. Headache may precede the development of pupil edema.
Vomiting
It may be present with or without nausea and invariably accompanies headache. Vomiting is present in two thirds of all cases of intracranial tumor but is absent in patients of intracranial tumors who do not have signs of raised intracranial tension.
Pupil edema or choked disc
It is the most important sign of raised intracranial tension. The earliest changes are increased redness of the disc with disappearance of the physiological cup. As the process increases the whole margin of the disc becomes lost. The venous congestion leads to hemorrhages and with outpouring of much exudation, the optic disc contracts leading to optic atrophy. In early stages of pupil edema, vision is not effected but subsequently depending on the degree of swelling, exudates and length of duration of pupil edema, vision becomes impaired and even blindness may result.
Pupil edema in cases of Intracranial tumors (Brain tumors) is always bilateral but it may appear in one eye before the other.
Giddiness
It is present in tumors of cerebellum or in tumors situated below the tentorium. It is often a feeling of unsteadiness or faintness. Mental drowsiness and Dullness with loss of vivacity may be an early important sign. As the disease progresses patient complains of heaviness and drowsiness. There is progressive decline in cognitive abilities and speech, gait or memory may be affected.
Diplopia. It is an important symptom and is experienced on looking to one or both sides. It is usually intermittent in the beginning of the disease.
Blood pressure pulse rate. Rising intra cranial pressure leads to fall in pulse rate and is characteristically seen in patients with rapid cerebral compression. There is also a rise in blood pressure levels while respiration may wax and wane and even gets depressed.
Seizures
Adult onset seizures are the commonest sign of raised intracranial pressure. These are like those of idiopathic epilepsy. Any person after the age of 30 who presents with onset of epileptic seizures must be evaluated for space occupying lesion in the brain.
Focal neurological signs
These may reflect the particular anatomic site of the tumor. A tumor in the sensory motor area has the highest incidence of epileptic fits while tumors of the pituitary produce characteristic endocrinal changes as well as visual field changes. Masses in the temporal lobe produce personality changes and cerebellar and brainstem lesions lead to in coordination with cranial nerve palsies. An acoustic neuroma growing in the cerebellopontine angle will result in cerebellar ataxia along with cranial nerve palsies.
False localizing signs
In cases of raised intracranial pressure the signs and symptoms which appear early are of great localizing value as compared to those signs which appear later and are due to shift of the intracranial contents resulting in shifting of the brain stem and stretching of nerves in its course. This results in cranial nerve palsies such as that of 3rd, 6th and seventh cranial nerves. If these palsies appear early in the course of disease, these shall indicate a brain stem lesions while if they appear in later course of disease, their importance is diminished and indicate only raised intracranial pressure. These are false localizing signs indicative of shift of the brain.
Nasal irritation
It is a peculiar symptom seen in a case of space occupying lesion where patient rubs his/her nose to relieve itching even when lying. The cause of this is not known.
Physical examination of the patient with suspected intracranial tumor. Any patient suspected of an Intracranial tumors should be thoroughly examined for presence of neurofibroma of the skin, hepatic enlargement, lymphadenopathy and a rectal examination / pelvic examination in females to exclude any malignancy. Besides this a complete record be maintained for any personality changes, neurological deficit, localizing signs and fundus examination. Careful examination of the skull may reveal thickening of bone, dilated blood vessels or areas of tenderness. Auscultation may reveal an audible bruit in a vascular tumor.
Investigations
Plain X-ray skull may reveal changes suggestive of raised intracranial tension, areas of local absorption of bone, enhanced vascular markings or areas of abnormal calcification (Tuberculoma, cysticercosis, oligodendroglioma). One should look for enlargement or destruction of sella turcica which is seen in intrasellar tumors.
CT Scan with contrast enhancement is the most important investigation. It shall not only reveal the size and site of the tumor but as well as associated edema.
MRI is preferred when a tumor is small and may not be visualized well with CT scan. Moreover turn ours in the posterior fossa, brain stem and cerebellum are visualized in greater detail by MRI.
Cerebral angiography – It is used to assess the anatomical relationship of major vessels to the tumor mass as well as its vascularily.
E.E.G. It was done previously to find abnormalities in the region of the tumor but now with the use of CT scan and MRI it has lost its value. Similarly ventriculography, a popular procedure earlier on has been discarded.
C.S.F. Examination is not of much help. Lumbar puncture is contraindicated in a case of Intracranial tumors as the procedure may be followed by herniation of cerebellar tonsils leading to sudden death.
In some cases technetium brain scan and gadolinium DPTA tests may be required to detect the suspicious tumor missed on CT scan and MN.